Adrian Kinnersley is a founder and expansion expert at In2America, helping international companies establish and grow their U.S. presence with confidence. Drawing from firsthand experience, he understands the real-world challenges of hiring, compliance, and scaling across states. Through In2America’s purpose-built PEO and EOR model, Adrian and his team handle payroll, taxes, benefits, HR, and insurance, allowing overseas-based businesses to focus fully on growth while their U.S. operations run smoothly from day one.
If you’re relocating to the U.S. as an international founder, tech worker, or startup team member, navigating the American healthcare system can feel like deciphering an entirely new language. Unlike many countries with public healthcare systems, the U.S. operates primarily on a private insurance model and understanding how to protect your health (and your wallet) is essential from day one.
In this post, we’ll break down the basics of U.S. healthcare and answer the most frequently asked questions from visa holders, expats, and startup founders entering the American market.
Technically, you are not legally required to have health insurance to reside in the U.S. unless you're in a state like Massachusetts, California, or New Jersey, which have costly state penalties associated with not being insured. However, not having insurance can be financially devastating if you get sick or injured without coverage.
A simple emergency room visit can cost $2,000–$10,000+ without insurance, and even routine procedures can quickly become unaffordable.
If you're:
…you absolutely should have coverage in place as soon as you arrive.
The U.S. system is insurance-driven and largely privatized. Here’s the simplified breakdown:
The best option depends on your visa type, employment status, and length of stay. Here are the main categories:
If your U.S. employer offers benefits, you’ll likely be eligible for a group health plan, which usually includes:
These plans offer better coverage at lower costs than individual plans, and are often partially subsidized by the employer
If you're self-employed, between jobs, or don’t have access to employer benefits, you can buy insurance via Healthcare.gov or your state exchange.
These plans are:
If you’re only staying for a few months and don’t need full U.S. coverage, consider short-term health insurance or travel medical plans. But beware:
Tip: Startup founders can access group plans through a PEO (Professional Employer Organization) even with just 1–5 employees. In2America specializes in helping international teams access affordable group health insurance from day one.
In many cases yes, especially for full-time W-2 employees. Most U.S. companies with more than 50 employees are required to provide “affordable” health insurance under the ACA.
Here's what you can typically expect:
If you’re employed through a PEO (like In2America), you’ll often get Fortune 500-style benefits even if your startup is small.
Caution: Contractors (1099 workers) are not typically eligible for employer health plans. You’ll need to secure your own insurance.
When you enroll in a U.S. health insurance plan—either through an employer, the ACA marketplace, or a PEO you’ll typically choose from different plan “types.” Each type offers a different balance of flexibility, cost, and provider access.
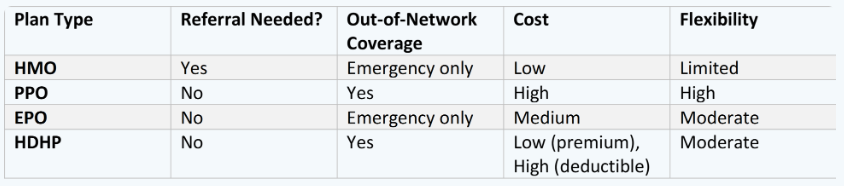
Here are the four most common types:
Best for: People who want predictable costs and are okay with less provider flexibility.
Best for: People who want freedom to choose their own doctors and are willing to pay more for it.
Best for: People who want some freedom without the high costs of a PPO.
Best for: Healthy individuals or families who rarely go to the doctor, aren’t on recurring prescription drugs, and want to save on premiums.
Pro Tip for International Founders: Many employees in the U.S. are unfamiliar with these acronyms too. When offering health plans, educate your team on their options. If you’re using a PEO like In2America, you can get help explaining plan types and selecting the best mix for your team.
COBRA stands for the Consolidated Omnibus Budget Reconciliation Act. It allows individuals who lose their job—or their health coverage due to quitting or being laid off—to continue their group health insurance for up to 18–36 months.
Key facts:
For visa holders, COBRA can help maintain health coverage while transitioning between employers or waiting for a new visa approval—but it’s not a long-term solution due to cost.

Health insurance in the U.S. isn’t just a nice-to-have—it’s a critical safety net. For international founders, remote employees, and expats entering the U.S., the right insurance plan can be the difference between thriving and financial disaster.
If you’re launching a U.S. entity or building a small team, a PEO partner like In2America can provide access to elite benefits, handle compliance, and reduce your HR burden, with no minimum employee headcount required
Visit In2America’s website to discover how their team helps international businesses hire, stay compliant, and scale confidently in the United States, without getting buried in payroll, taxes, or HR complexity.